What is Prevention?
- Home
- About Prevention
- About Prevention
- What is Prevention?
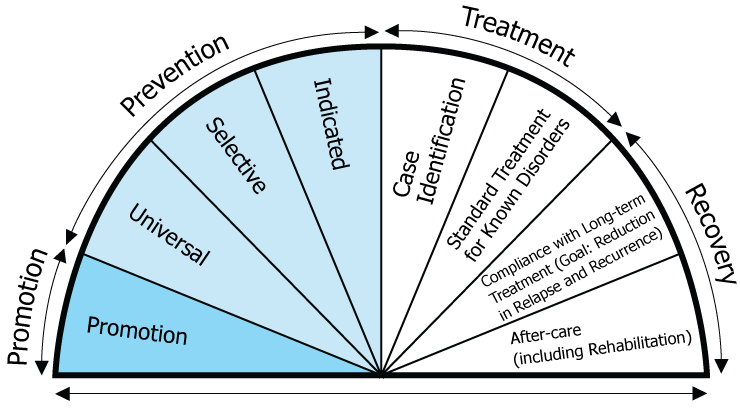
Most people think of ‘substance use prevention’ as efforts that help an individual avoid developing a substance use disorder, also known as addiction. And while a major goal of prevention is to reduce the number of people who experience addiction, prevention occurs at different levels and can occur even after a person has used a substance. This is illustrated in the Behavioral Health Continuum of Care Model which identifies several levels at which it is possible to intervene to prevent or reduce the progression of a substance use disorder. It is referred to as the Behavioral Health Continuum of Care because it captures the levels of prevention that address behavioral health, which includes both substance use and mental health.
The continuum of care includes:
- Promotion: Efforts that broadly promote healthy behaviors.
- Prevention: Efforts that aim to prevent or reduce the risk of potentially problematic behaviors, such as underage drinking. Prevention activities can target whole populations that have not yet engaged in the targeted behavior (universal), subsets of those populations that are at risk for the behavior (selective), or even smaller subsets that have already started to engage in the behavior and for which early intervention could help reduce the progression of the behavior (indicated).
- Treatment: Services that are designed to assist individuals who experience a behavioral health disorder so that they are able to lead healthy, productive lives. Treatment does not necessarily mean that a person’s mental health or substance use disorder is ‘cured.’ Like treatment approaches for other chronic diseases, behavioral health treatment generally includes a combination of interventions that assist an individual in managing their behavioral health disorder so that it does not interfere with their ability to meet their basic needs and develop healthy relationships with others.
- Recovery: Services that assist a person who has already received treatment
Why is prevention important?
Most people understand that preventing substance use disorders is a positive thing. Prevention can decrease the human costs of addiction, allowing individuals to be mentally and physically healthy, connected to their families, and capable of meeting their responsibilities in society. Beyond that, however, the U.S. Substance Abuse and Mental Health Services Administration (SAMHSA) points out that prevention also saves society money. The Institute of Medicine and National Research Council’s Preventing Mental, Emotional, and Behavioral Disorders Among Young People report – 2009 notes that cost-benefit ratios for early treatment and prevention programs for addictions and mental illness programs range from 1:2 to 1:10. This means a $1 prevention investment leads to $2 to $10 savings in health costs, criminal and juvenile justice costs, educational costs, and lost productivity. So we all win when prevention is a foundational part of our approach to addressing addiction.
Risk and Protective Factors
Each person carries with them a varying degree of risk that they could experience a substance use disorder. The factors–known as risk factors–can occur at the biological, psychological, family, community or cultural level. For instance, risk factors can include a family history of addiction, mental health disorders like depression or anxiety, insecure relationships with parents/caregivers, or limited access to healthcare or economic and educational opportunities in a community.
Researchers have identified a series of ten risk factors that are particularly impactful and can increase the risk of violence or addiction in a young person. Known as Adverse Childhood Experiences, or ACEs, these risk factors are more common than many people realize. You can view the ten ACE questions here to calculate your own ACE score. Keep in mind that ACEs are not prescriptive. Their presence does not mean that a person will experience addiction; it just means that they have a higher risk for addiction. Additionally, the Partnership for Drug Free Kids has developed a helpful overview as to why some teens use alcohol and other drugs.
Fortunately, protective factors can also exist to varying degrees for each person and can reduce the impact of risk factors. For example, a child who grows up in a home where substance use is not frequent or who has a loving, secure relationship with a parent/caregiver has a lower risk for addiction and other potentially unhealthy behaviors. Those protective factors might be strong enough to outweigh the impact of risk factors such as an unsafe neighborhood or limited financial security.
The Search Institute has conducted decades of research about factors that can boost a person’s resiliency, organizing them into the developmental assets framework. The 40 developmental assets that the Search Institute has identified include external factors like support, empowerment, boundaries and expectations, and constructive use of time; internal factors exist in domains like commitment to learning, positive values, social competencies and positive identity. The good news is that because half of the developmental assets are external, parents, families, schools and communities have the power to positively impact those factors. You can download free copies of the developmental assets for various age groups (available in English and Spanish) at the Search Institute website.
It is worth noting that some risk and protective factors, like genetics, are fixed and therefore do not change over time. Other risk and protective factors are considered variable because they can change over the course of a person’s life. These include income level, peer group, and educational or employment status. As a result, a person’s risk for addiction and other behaviors should be periodically assessed and should not assumed to be static.